Understanding Vasculitis: Wegener’s Granulomatosis and Microscopic Polyangiitis (MPA) Explained
Vasculitis refers to a group of rare autoimmune disorders where the body’s immune system mistakenly attacks blood vessels, causing inflammation, narrowing, or even destruction of these vessels. Among the many forms of vasculitis, Wegener’s Granulomatosis (now called Granulomatosis with Polyangiitis, GPA) and Microscopic Polyangiitis (MPA) are two closely related but distinct conditions. Both can affect small- and medium-sized blood vessels and, if untreated, may lead to serious organ damage. At IRIS Clinics, our rheumatology experts specialize in early diagnosis and treatment of these conditions to prevent complications and improve outcomes.
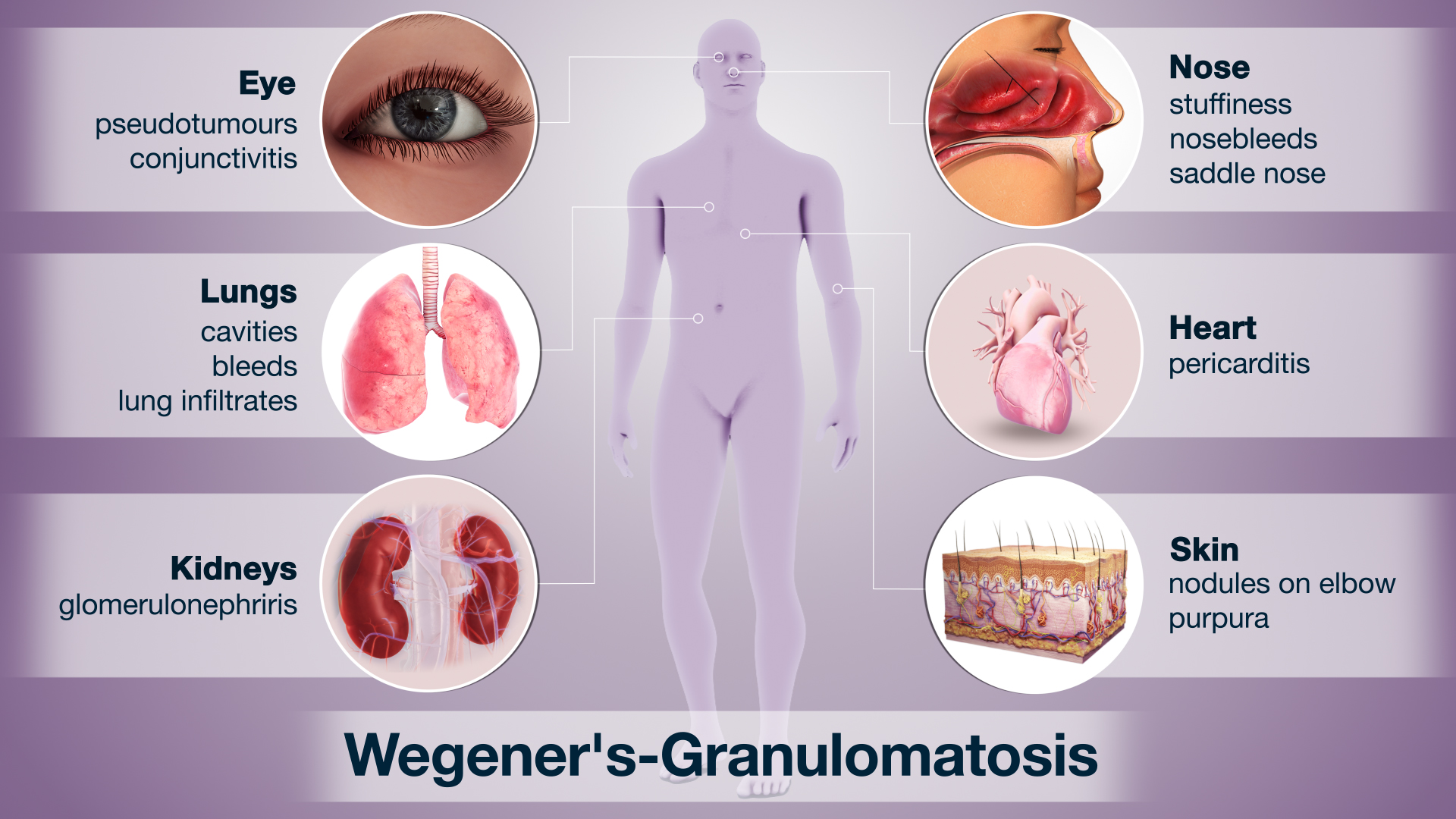
Unlike common joint diseases, vasculitis affects not only joints but also vital organs such as the lungs, kidneys, skin, and nerves. The inflammation disrupts normal blood flow and can lead to tissue damage. Wegener’s Granulomatosis is characterized by granulomas (clusters of immune cells) and often affects the sinuses, lungs, and kidneys. MPA, on the other hand, typically spares the upper respiratory tract but commonly involves the kidneys and lungs. Both conditions are considered ANCA-associated vasculitides, meaning they are linked to antibodies that target neutrophils, a type of white blood cell.
Early recognition of GPA and MPA symptoms is crucial. At IRIS Clinics, we use advanced blood tests, imaging, and biopsies to confirm diagnosis, enabling timely treatment and better long-term control.
Symptoms of these conditions vary widely and often mimic other diseases, making diagnosis challenging. Common early signs include unexplained fever, fatigue, weight loss, and muscle or joint pain. Wegener’s Granulomatosis often presents with sinus infections, nasal congestion, nosebleeds, coughing, or chest pain, while MPA frequently causes shortness of breath, coughing up blood, and signs of kidney dysfunction such as blood in the urine. Both can cause skin rashes, nerve pain, or numbness due to nerve inflammation.
Since GPA and MPA can progress rapidly, timely intervention is essential. At IRIS Clinics, our multidisciplinary approach includes rheumatologists, nephrologists, and pulmonologists to ensure all affected organs are evaluated and treated. We emphasize early use of immunosuppressive medications like corticosteroids, rituximab, or cyclophosphamide to control inflammation and prevent irreversible damage.
Key Features of GPA and MPA
Here’s a closer look at how these conditions typically present and differ:
1. Wegener’s Granulomatosis (GPA)
- Granulomas and inflammation in the upper respiratory tract (sinus, nose, throat).
- Lung involvement with nodules, coughing, chest discomfort, or hemoptysis.
- Kidney inflammation (glomerulonephritis) leading to protein or blood in urine.
- Eye and ear complications, sometimes causing hearing loss or vision problems.
2. Microscopic Polyangiitis (MPA)
- More likely to involve kidneys and lungs without granulomas.
- Respiratory symptoms such as coughing and shortness of breath.
- Can cause nerve pain, tingling, or weakness due to peripheral nerve involvement.
- Skin rashes or ulcers caused by small-vessel inflammation.
3. Shared Symptoms
- Fever, fatigue, weight loss, and general malaise.
- Muscle and joint aches, sometimes mistaken for arthritis.
- ANCA-positive blood tests in most cases, aiding diagnosis.
Treatment is personalized based on the severity and organs involved. Maintenance therapy with immunosuppressants helps prevent relapses, while supportive care includes blood pressure control, kidney monitoring, and infection prevention. At IRIS Clinics, we combine medication with lifestyle guidance, helping patients manage fatigue, maintain organ health, and return to daily activities with confidence.