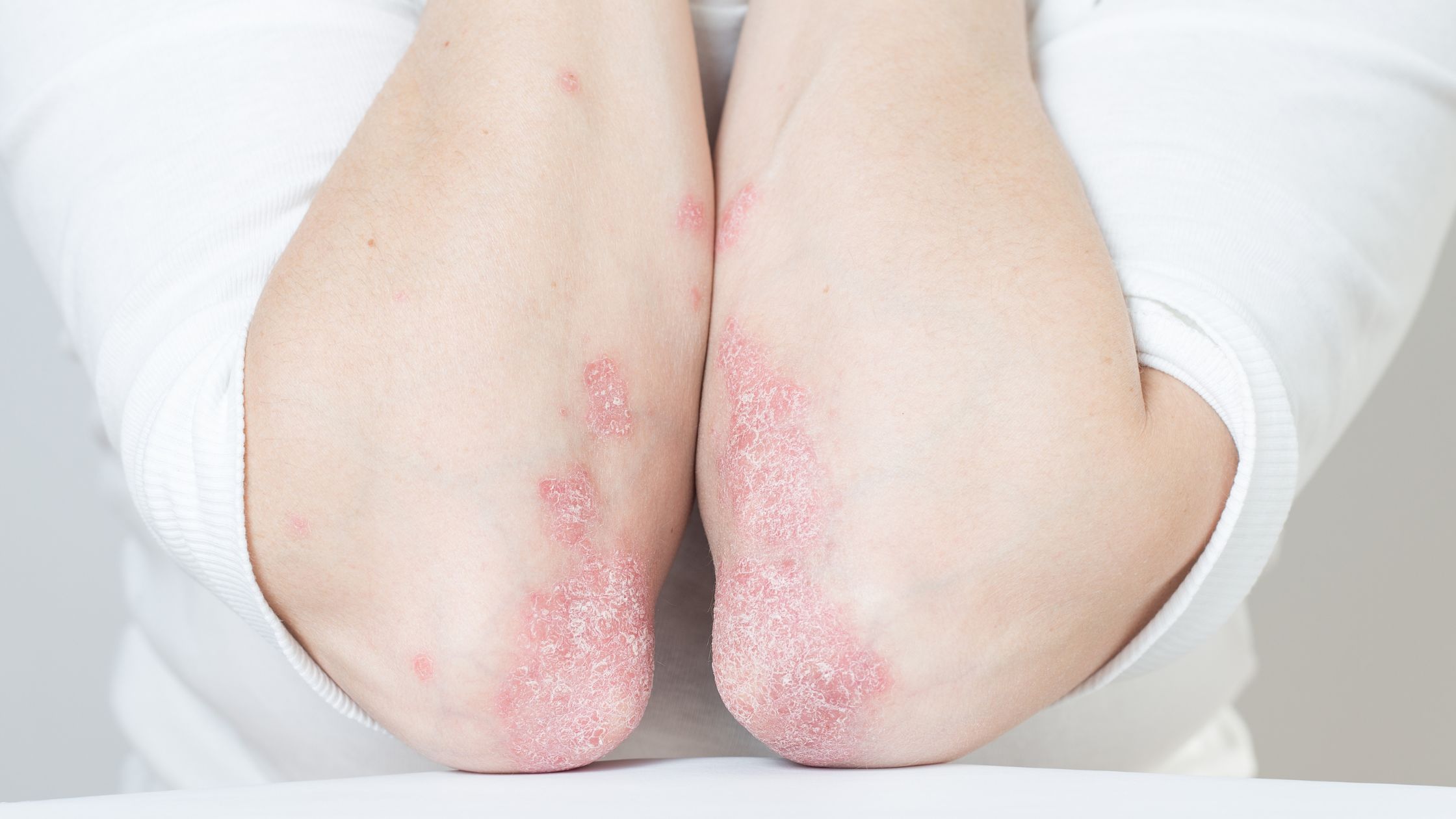
Psoriatic Arthritis and Skin Psoriasis: How Are They Connected?
Psoriatic Arthritis (PsA) is a chronic inflammatory condition that uniquely combines joint disease with skin symptoms. While psoriasis is known for causing red, scaly patches on the skin, PsA involves inflammation of the joints and connective tissues, often appearing in people who already have psoriasis. At IRIS Clinics, we regularly treat patients who first notice psoriasis symptoms on the skin and later experience joint discomfort, highlighting the strong link between these two conditions. Early detection is crucial to prevent long-term joint damage and improve quality of life.
Unlike other forms of arthritis, PsA arises when the immune system mistakenly attacks both skin cells and joint tissues. This autoimmune response leads to overproduction of skin cells and chronic joint inflammation. Without timely management, PsA can cause progressive cartilage and bone damage, resulting in stiffness, swelling, and even permanent deformities. The presence of psoriasis increases the risk of PsA, but not everyone with skin psoriasis develops arthritis, making routine monitoring essential.
Understanding the connection between psoriasis and PsA is vital. At IRIS Clinics, our integrated dermatology and rheumatology expertise ensures patients receive comprehensive care. We use advanced imaging, lab tests, and clinical evaluation to detect PsA early and design customized treatment plans that target both skin and joint health.
Symptoms vary depending on the severity and areas affected. PsA commonly causes joint pain, stiffness, and swelling, especially in fingers, toes, and large joints like knees and ankles. Skin lesions often appear on the scalp, elbows, knees, and nails, which may show pitting or thickening. Nail changes are particularly significant as they can indicate an increased risk of PsA. Unlike rheumatoid arthritis, PsA can affect joints asymmetrically, meaning one side of the body may be more affected than the other.
Flare-ups can be unpredictable, with periods of intense symptoms followed by remission. Some patients experience enthesitis (inflammation where tendons attach to bone) or dactylitis (swelling of entire fingers or toes, sometimes called “sausage digits”). These signs, along with fatigue and eye inflammation (uveitis), underline the systemic nature of PsA. Regular checkups at IRIS Clinics, combined with imaging like ultrasound and MRI, are essential for early diagnosis and preventing complications.
How Psoriasis and PsA Affect the Body
Here’s how these conditions often manifest together:
1. Skin and Nails
- Psoriasis usually appears as thick, red, scaly patches on the skin.
- Nails may show pitting, thickening, or separation from the nail bed.
- These visible changes are often the first signs, but may also signal future joint issues.
2. Joints and Tendons
- Pain, stiffness, and swelling in small and large joints.
- Dactylitis causes entire fingers or toes to swell.
- Enthesitis may lead to tenderness in heels, elbows, or spine.
3. Systemic Impact
- Fatigue, eye inflammation, and cardiovascular risks are more common in PsA.
- PsA may increase the risk of metabolic syndrome and other autoimmune conditions.
- Early treatment helps reduce long-term risks and preserve overall health.
At IRIS Clinics, our approach to PsA care involves more than just symptom management. We combine disease-modifying medications, biologic therapies, lifestyle planning, and physiotherapy to help patients maintain mobility, reduce skin flare-ups, and protect joints. Coordinated care between dermatologists and rheumatologists ensures that patients receive holistic support for both the visible skin symptoms and the less obvious joint inflammation.