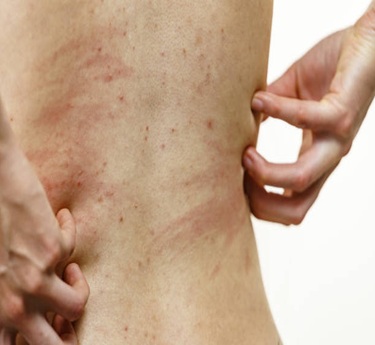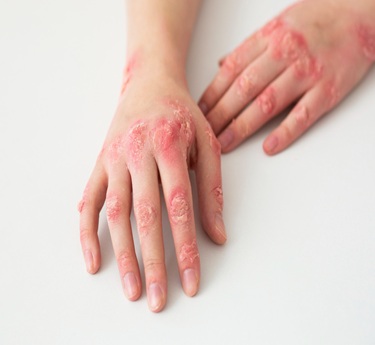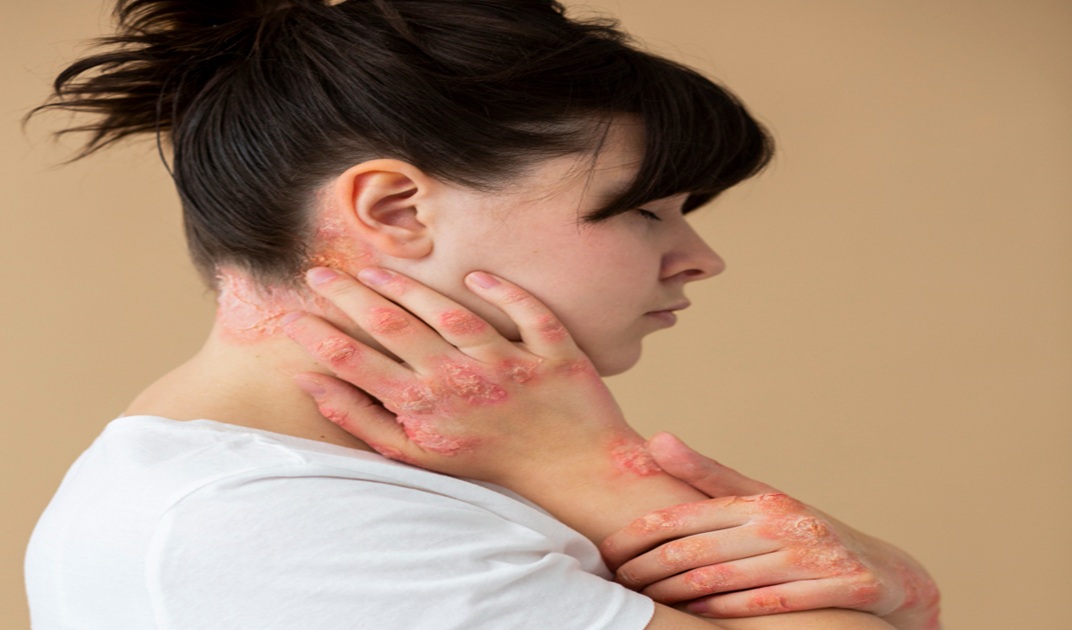
Dermatomyositis is a rare inflammatory autoimmune disease that primarily affects the skin and muscles. It causes progressive muscle weakness and distinctive skin rashes, most commonly over the face, chest, knuckles, and shoulders. The condition can affect both adults and children but is more common in women between 40 and 60 years of age. If left untreated, it can lead to difficulty performing daily activities. Its cause is unknown, but genetic and immune factors are believed to play a role. Early diagnosis is key to reducing complications and improving function.
Additional symptoms may include trouble climbing stairs, fatigue, difficulty swallowing, or shortness of breath. Treatment typically includes corticosteroids, immunosuppressants, and physical therapy. Skin care may involve sun protection and topical treatments. Ongoing monitoring is essential to adjust medications, evaluate organ involvement, and support long-term strength and mobility.
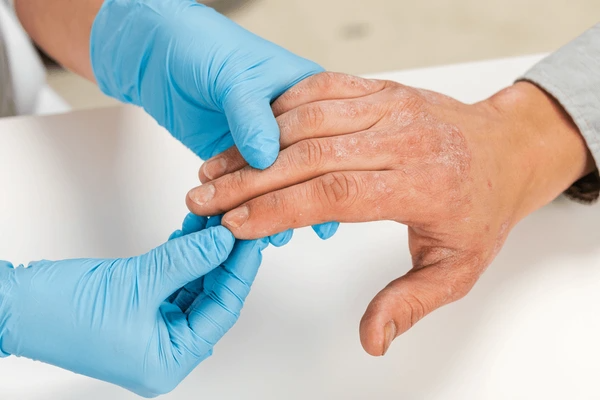
Dermatomyositis is an inflammatory autoimmune condition that affects both the skin and muscles, leading to characteristic rashes and progressive muscle weakness if not treated early.
Diagnosing Dermatomyositis involves evaluating muscle weakness, distinctive skin rashes, and confirming inflammation through blood tests, imaging, and sometimes biopsy.
Although there is no cure for Dermatomyositis, timely and tailored treatments can help reduce inflammation, restore muscle strength, and improve skin symptoms over time.
Rehabilitation therapies and supportive interventions play a key role in restoring strength, managing fatigue, and improving quality of life in Dermatomyositis.