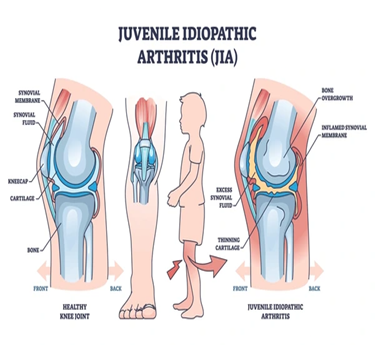
Paediatric Rheumatology focuses on diagnosing and treating autoimmune and inflammatory conditions affecting children’s joints, muscles, and connective tissues. One of the most common conditions is Juvenile Idiopathic Arthritis (JIA), which can cause persistent joint pain, swelling, stiffness, and fatigue. These disorders often affect mobility, growth, and quality of life in children, requiring early attention.
Early diagnosis is crucial to managing symptoms and preventing long-term joint damage. Treatment options include non-steroidal anti-inflammatory drugs (NSAIDs), disease-modifying antirheumatic drugs (DMARDs), physical therapy, and lifestyle modifications. In more severe cases, biologic therapies may be used. Ongoing care with a paediatric rheumatologist is essential for monitoring growth, ensuring joint health, and improving overall well-being.
Explore common juvenile autoimmune diseases, each with unique symptoms and treatment approaches. Swipe to learn more about each condition.
Paediatric Rheumatology deals with autoimmune and inflammatory disorders in children, affecting joints, muscles, and connective tissues. Early diagnosis is key to preventing long-term joint damage and supporting healthy development.
Diagnosing paediatric rheumatologic conditions involves a detailed medical history, physical examination, and specialized tests to identify inflammation, autoimmunity, or joint involvement. Early detection is crucial for effective treatment and preventing long-term complications.
Treatment in Paediatric Rheumatology aims to control inflammation, relieve pain, and preserve joint function and quality of life. A multidisciplinary approach involving medications, therapy, and lifestyle modifications is often recommended.
Supportive care in Paediatric Rheumatology focuses on reducing symptoms, improving joint function, and enhancing the child’s overall well-being through integrated therapy, education, and emotional support.