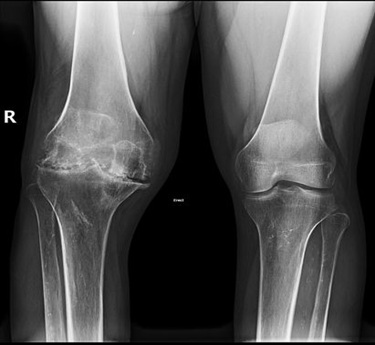
Haemophilic Arthropathy is a joint condition that results from repeated bleeding into the joints, commonly seen in individuals with haemophilia. Over time, this bleeding damages the cartilage and joint lining, leading to pain, stiffness, and reduced mobility. The most commonly affected joints include the knees, elbows, and ankles. The condition typically begins in childhood for those with moderate to severe haemophilia and progresses without proper treatment. Unlike inflammatory arthritis, haemophilic arthropathy is caused by mechanical damage due to bleeding episodes. Early treatment and preventive care can help reduce joint damage and preserve function.
While joint damage from haemophilic arthropathy is not reversible, management strategies can reduce pain and improve mobility. These include factor replacement therapy, physiotherapy, and in some cases, surgery. Regular monitoring and early intervention are essential to prevent progression and maintain quality of life.
Haemophilic Arthropathy is a chronic joint condition caused by repeated bleeding into joints, commonly seen in people with moderate to severe haemophilia.
Diagnosing Haemophilic Arthropathy involves assessing joint history, clinical examination, imaging, and blood tests in individuals with known haemophilia and recurrent joint bleeds.
Haemophilic Arthropathy requires a combination of preventive care, joint protection strategies, and medical management to reduce pain, preserve mobility, and avoid joint damage.
Supportive therapies and long-term care are essential for managing pain, improving joint function, and enhancing quality of life in individuals with Haemophilic Arthropathy.