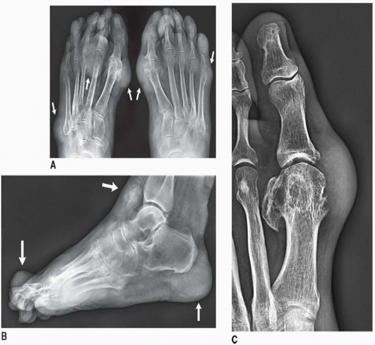
Metabolic Arthropathies are joint disorders caused by abnormalities in the body’s metabolism, most commonly due to crystal deposits such as uric acid (gout) or calcium pyrophosphate (CPPD/pseudogout). These deposits trigger inflammation in the joints, leading to sudden pain, swelling, and redness. Gout often affects the big toe, while pseudogout may involve the knees, wrists, or ankles. These conditions are more common in middle-aged and older adults and may be associated with other metabolic conditions like diabetes or kidney disease. Unlike autoimmune arthritis, metabolic arthropathies are driven by biochemical imbalances, and flare-ups can be intense and disabling if not managed appropriately.
Although symptoms may come and go, metabolic arthropathies can cause long-term joint damage if left untreated. Management focuses on reducing inflammation during attacks and lowering crystal levels through medications and dietary changes. With proper care—including uric acid control, lifestyle modification, and follow-up—most patients can lead active, pain-free lives and avoid future joint complications.

Metabolic Arthropathies are joint disorders caused by the buildup of metabolic crystals like uric acid or calcium pyrophosphate, leading to painful inflammatory episodes.
Diagnosing Metabolic Arthropathies involves clinical evaluation, joint fluid analysis, blood tests, and imaging to detect crystal deposits and rule out other joint diseases.
Metabolic Arthropathies are managed through medications, lifestyle changes, and supportive care to control inflammation, prevent crystal formation, and protect joint health.
Supportive therapies play a vital role in managing pain, preventing joint stiffness, and maintaining function in people living with Metabolic Arthropathies.