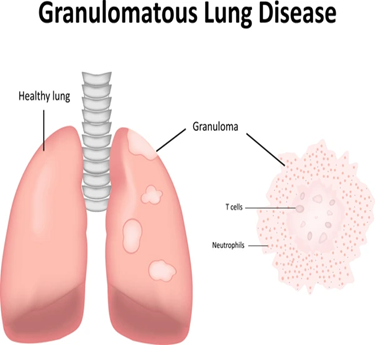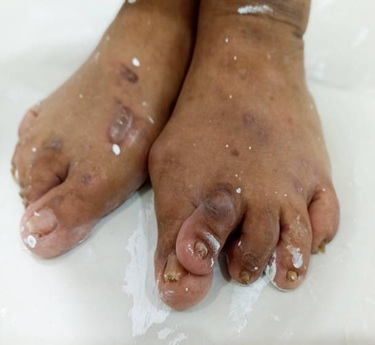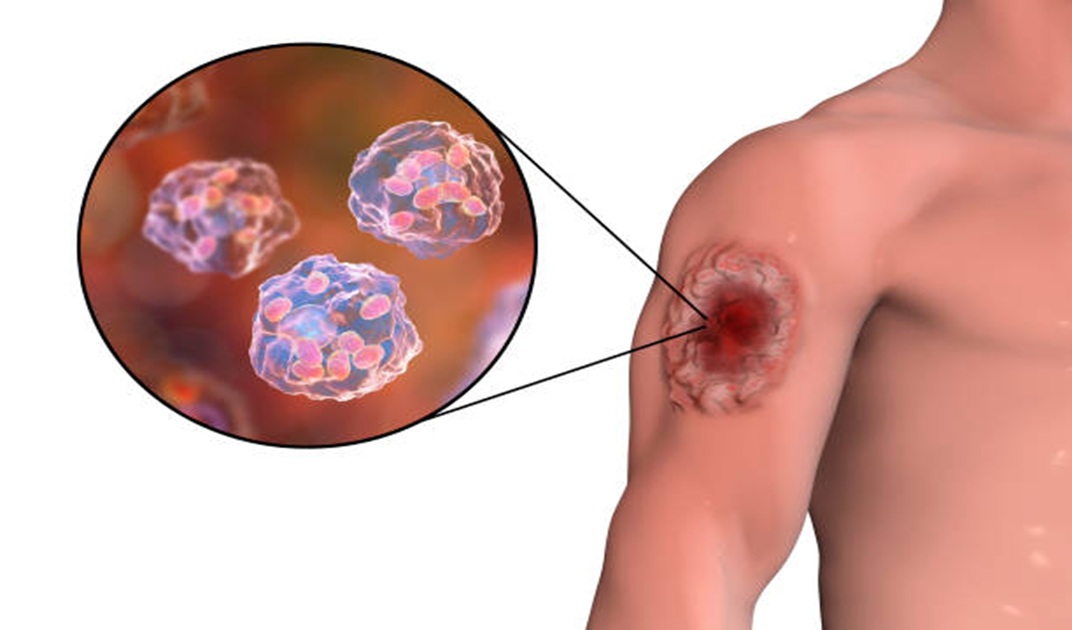
Wegener's Granulomatosis (now called Granulomatosis with Polyangiitis - GPA) and Microscopic Polyangiitis (MPA) are rare autoimmune vasculitic diseases that cause inflammation of small to medium-sized blood vessels. These conditions can affect organs such as the lungs, kidneys, sinuses, and skin. GPA often presents with sinus issues, cough, and nosebleeds, while MPA commonly leads to kidney problems and fatigue. Early diagnosis is critical to reduce organ damage and improve outcomes through timely treatment.
Common symptoms may include chronic sinusitis, shortness of breath, persistent cough, hematuria (blood in urine), skin rashes, and joint pain. Treatment generally involves high-dose corticosteroids and immunosuppressants like cyclophosphamide or rituximab. In some cases, plasma exchange may be used. Regular monitoring is essential to manage disease activity, prevent relapses, and minimize medication side effects, helping patients maintain long-term health and quality of life.
Wegener’s Granulomatosis (GPA) and Microscopic Polyangiitis (MPA) are rare autoimmune vasculitides causing inflammation in blood vessels and affecting vital organs like lungs and kidneys.
Diagnosing Wegener’s Granulomatosis and Microscopic Polyangiitis involves clinical evaluation, laboratory tests, imaging, and sometimes biopsy to confirm small-vessel vasculitis and organ involvement.
Although there is no cure for GPA or MPA, aggressive treatment can reduce inflammation, prevent relapse, and protect organs from long-term damage.
Supportive therapies and long-term care play a key role in managing fatigue, restoring function, and improving quality of life in GPA and MPA.