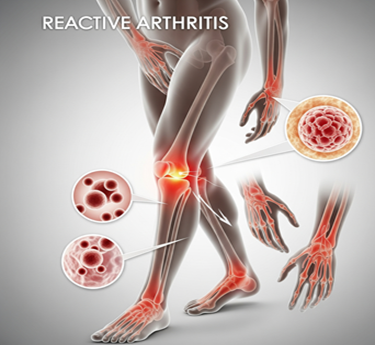
Reactive Arthritis is a type of inflammatory arthritis that develops in response to an infection, typically in the urinary tract, genitals, or intestines. It most often affects the joints, eyes, and urinary tract. The condition is more common in men between the ages of 20 and 40. Symptoms may include joint pain, swelling, and redness, especially in the knees, ankles, and feet. It is not contagious, but is triggered by a prior infection. Bacterial infections such as chlamydia or salmonella are common causes. Without proper care, reactive arthritis can become chronic or lead to joint stiffness and discomfort.
Other symptoms may include painful urination, eye redness, skin rashes, or heel pain. Early diagnosis and treatment with anti-inflammatory drugs, antibiotics, and physical therapy can relieve symptoms and prevent complications. Ongoing monitoring is important to manage flares and preserve joint function and mobility.
Reactive Arthritis is a type of autoimmune arthritis that develops after certain infections, affecting the joints, eyes, and urinary tract, and may cause inflammation, discomfort, and complications if untreated.
Diagnosing Reactive Arthritis can be difficult, as its symptoms overlap with others.
While Reactive Arthritis cannot be cured, timely treatment can reduce pain and control inflammation.
Physical therapy and, in some cases, surgery can restore mobility, ease pain, and address joint-related damage.