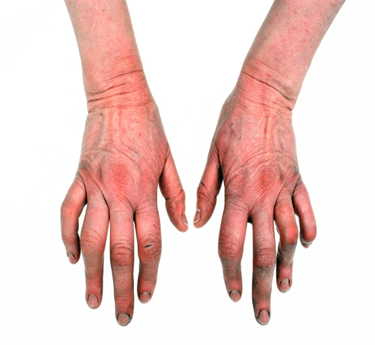
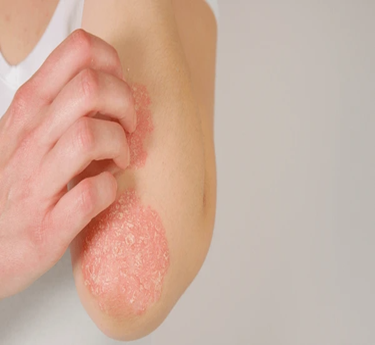
Psoriatic Arthritis is a chronic autoimmune condition that affects some people who have psoriasis, a skin disease that causes red, scaly patches. It most commonly impacts the joints and areas where tendons attach to bones. The disease typically appears in adults between 30 and 50 years of age. Symptoms may include joint pain, swelling, and stiffness, often in the fingers, toes, knees, or spine. Psoriatic arthritis is not contagious, but it can severely affect mobility if untreated. Both genetic and immune factors play a role in the disease. Early care is essential to reduce inflammation and joint damage.
Other symptoms may include nail changes, fatigue, morning stiffness, or swollen fingers. Early diagnosis and treatment with anti-inflammatory drugs, DMARDs, and biologics can help manage symptoms and prevent permanent damage. Regular follow-ups help monitor disease activity, adjust treatment, and protect joint health and daily function.

Psoriatic Arthritis is a type of inflammatory arthritis linked to psoriasis, affecting the joints, skin, and tendons, and may lead to pain, stiffness, and long-term joint issues if untreated.
Diagnosing Psoriatic Arthritis can be challenging, as its signs often mimic other joint conditions.
While Psoriatic Arthritis cannot be cured, early intervention can reduce joint damage and improve daily function.
Physical therapy and, in some cases, surgery can restore mobility, ease pain, and address joint-related damage.