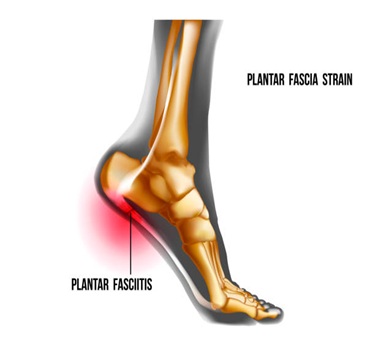
Plantar Fasciitis is a common condition that causes pain and inflammation in the plantar fascia, the thick band of tissue that connects the heel bone to the toes. It typically causes sharp heel pain, especially with the first steps in the morning or after periods of rest. The condition is more frequent in runners, people who are overweight, or those who wear improper footwear.
Early diagnosis helps in managing symptoms effectively and preventing chronic pain. Treatment options include rest, stretching exercises, orthotic support, physical therapy, and anti-inflammatory medications. In persistent cases, corticosteroid injections or advanced therapies like shockwave treatment may be recommended. Supportive footwear, weight management, and foot care are essential for long-term relief and preventing recurrence.
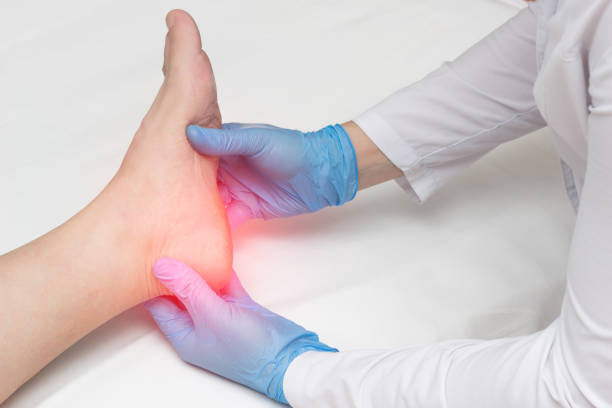
Plantar Fasciitis is an inflammation of the plantar fascia, a thick band of tissue running across the bottom of the foot. It causes heel pain and stiffness, especially with the first steps in the morning or after long periods of rest.
Diagnosing Plantar Fasciitis typically involves a clinical evaluation based on symptoms, physical examination, and sometimes imaging tests. Early diagnosis ensures effective pain relief and prevents chronic heel pain.
Treatment for Plantar Fasciitis focuses on relieving heel pain, reducing inflammation, and restoring normal foot function. A combination of conservative therapies, physical exercises, and supportive footwear is usually effective.
Supportive care for Plantar Fasciitis focuses on relieving pain, improving foot function, and preventing recurrence through targeted therapies, supportive footwear, and lifestyle adjustments.