Dermatomyositis Symptoms: Skin Rashes and Muscle Weakness Explained
Dermatomyositis (DM) is a rare autoimmune condition characterized by distinctive skin rashes and progressive muscle weakness. It can affect people of all ages but is most commonly diagnosed in adults between 40 and 60 and children between 5 and 15. At IRIS Clinics, we often see patients presenting with early skin changes or unexplained muscle fatigue, making timely recognition essential for diagnosis and management. The disease not only impacts the muscles and skin but may also involve the lungs, heart, and other internal organs, emphasizing the need for comprehensive care.
Unlike common rashes or muscle soreness caused by overuse, dermatomyositis occurs when the immune system mistakenly attacks healthy muscle fibers and skin cells. This leads to chronic inflammation, muscle fiber damage, and visible skin changes. Without proper treatment, DM can result in significant disability, reduced quality of life, and complications such as calcinosis (calcium deposits under the skin) or interstitial lung disease.
Understanding dermatomyositis symptoms early is crucial. At IRIS Clinics, our rheumatology and dermatology experts use advanced diagnostics, including blood tests, muscle enzyme studies, EMG (electromyography), skin and muscle biopsies, and MRI scans to detect inflammation, confirm diagnosis, and guide personalized treatment for long-term outcomes.
The hallmark symptoms of dermatomyositis are a combination of muscle weakness and distinct skin rashes. Symptoms often appear gradually but can sometimes develop suddenly. The muscle weakness usually affects the proximal muscles those closest to the trunk of the body making daily activities such as climbing stairs, lifting objects, or getting up from a chair challenging. The skin symptoms can vary widely, from subtle rashes to striking purplish or reddish patches, often mistaken for allergic reactions or sunburn.
Early recognition and regular monitoring are key. At IRIS Clinics, we emphasize multidisciplinary care with rheumatologists, dermatologists, and physiotherapists working together to manage symptoms, reduce inflammation, and prevent complications. Advanced imaging and enzyme-level monitoring help track disease progression and treatment response accurately.
Key Dermatomyositis Symptoms in Skin and Muscles
Below are the hallmark signs and symptoms of dermatomyositis that patients and caregivers should look out for:
1. Skin Manifestations
- **Heliotrope Rash:** A violet or dusky rash around the eyes and eyelids, often with swelling.
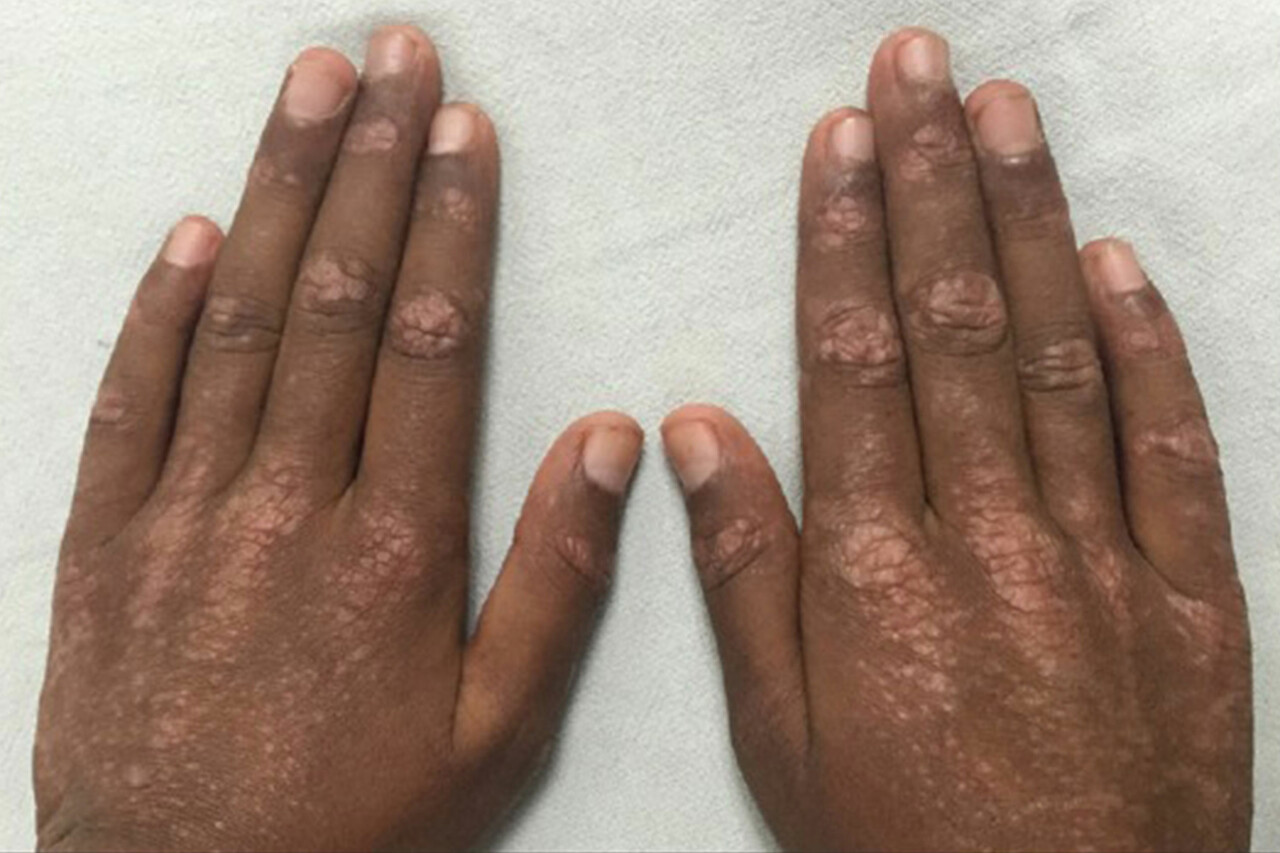
- **Gottron’s Papules:** Raised, scaly, reddish or violet bumps over the knuckles, elbows, and knees.
- **Photosensitive Rashes:** Rashes that worsen with sun exposure, appearing on the face, neck, shoulders, and upper back (shawl sign).
- **Nailfold Changes:** Redness and tiny blood vessel abnormalities around the nails.
- **Scalp and Hair Changes:** Some patients may experience scalp tenderness and hair loss in affected areas.
2. Muscle Involvement
- Progressive weakness in the shoulders, hips, thighs, and neck muscles.
- Difficulty with daily activities like rising from a seated position, lifting arms overhead, or climbing stairs.
- Muscle tenderness, soreness, or aching that may be mistaken for exercise fatigue.
- In severe cases, swallowing and breathing muscles may be affected, leading to dysphagia or respiratory complications.
3. Systemic Symptoms and Complications
- General fatigue and low-grade fever.
- Joint pain or stiffness, sometimes overlapping with other autoimmune conditions.
- Lung involvement, including interstitial lung disease causing cough and breathlessness.
- Calcinosis: Firm lumps of calcium deposits under the skin, particularly in children with juvenile dermatomyositis.
- Increased risk of malignancy in adult-onset dermatomyositis, requiring regular screening.
At IRIS Clinics, treatment is tailored based on the severity of symptoms and organ involvement. Therapies include corticosteroids to control inflammation, immunosuppressive drugs, biologics, physical therapy, and sun protection strategies for skin care. Nutrition and lifestyle modifications also play an important role in managing fatigue and improving muscle strength. With early and consistent treatment, many patients achieve remission or long-term disease control, significantly improving quality of life.