PAN Management: Latest Treatment Strategies and Care Guidelines
Polyarteritis Nodosa (PAN) is a rare but serious autoimmune condition that affects medium-sized arteries, leading to inflammation and damage in multiple organs. At IRIS Clinics, we emphasize the importance of early recognition and multidisciplinary care to manage PAN effectively. Symptoms can vary widely, often involving the skin, muscles, kidneys, nervous system, and gastrointestinal tract. Because PAN can progress rapidly without treatment, understanding its early warning signs and treatment options is essential for patients and caregivers.
Unlike common joint or muscle disorders, PAN is caused by the immune system mistakenly attacking healthy blood vessels, causing inflammation and restricted blood flow. Over time, this can result in tissue damage, organ dysfunction, and severe complications such as aneurysms or kidney failure. Without timely intervention, PAN can become life-threatening, making accurate diagnosis and long-term management crucial for better patient outcomes.
At IRIS Clinics, our rheumatology team uses advanced diagnostics such as blood tests, angiography, and biopsy to confirm PAN and assess disease activity. Tailored treatment strategies, including immunosuppressive therapies and organ-specific care plans, help patients achieve remission and protect long-term health.
Symptoms of PAN can differ greatly from person to person. Some patients experience persistent muscle pain, fatigue, and fever, while others may notice skin ulcers, nerve damage, or high blood pressure due to kidney involvement. Because these symptoms overlap with other autoimmune conditions, misdiagnosis is common. Regular follow-ups and comprehensive evaluation at a dedicated rheumatology center like IRIS Clinics are key to avoiding delays in treatment.
The condition can present suddenly with acute symptoms or develop gradually over months. Flare-ups may affect specific organs, requiring close monitoring and adjustment of medications. Our approach combines early aggressive therapy to control inflammation with long-term maintenance plans to reduce relapse risk and prevent complications.
Key Areas Affected by PAN and Their Management
PAN can impact various organs and systems. Here are the most commonly affected areas and strategies used at IRIS Clinics for optimal management:
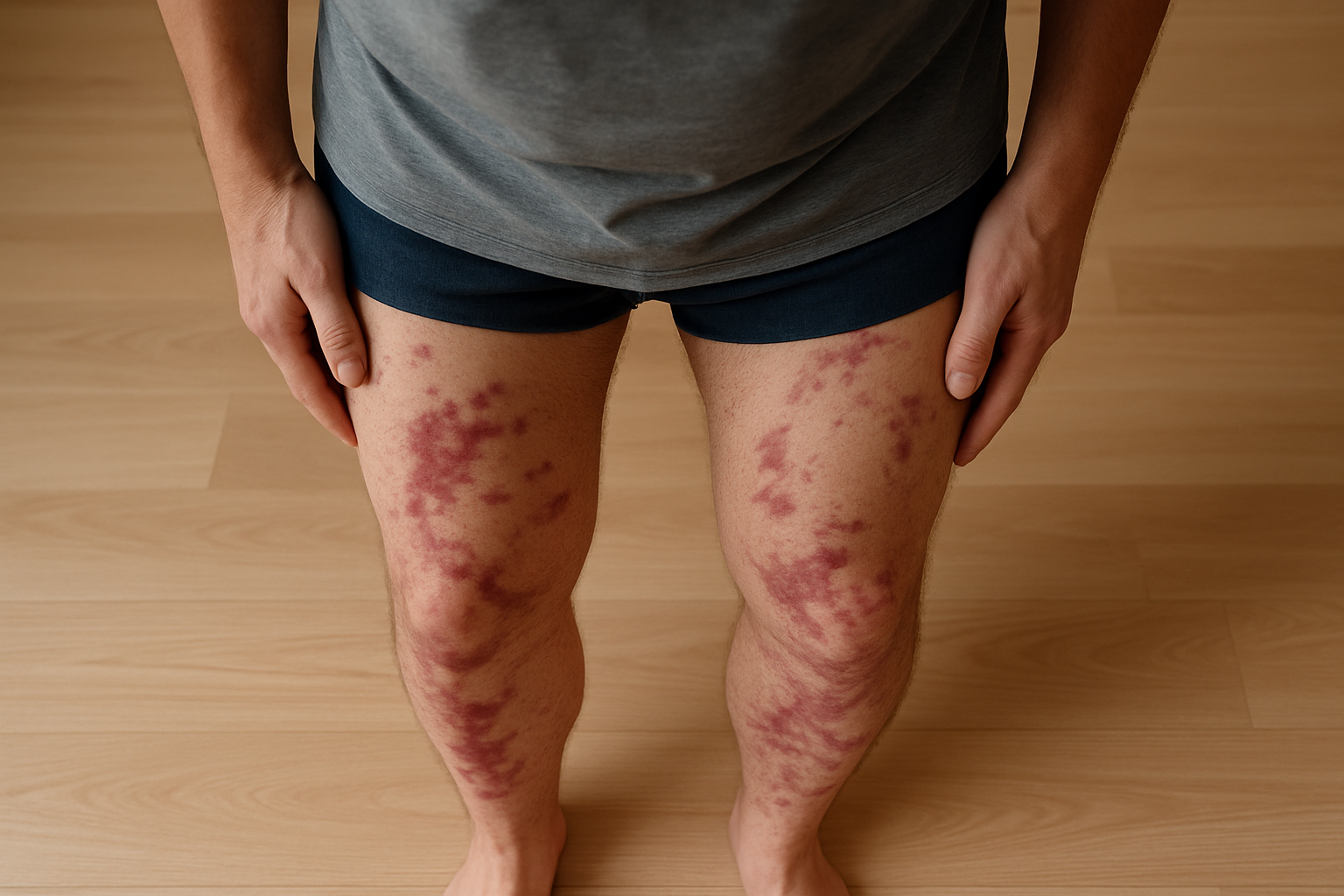
1. Skin and Muscles
- Painful skin nodules, ulcers, or rashes caused by inflamed blood vessels.
- Muscle weakness or persistent myalgia due to restricted blood flow.
- Early corticosteroid therapy and topical care help relieve symptoms and promote healing.
2. Kidneys
- High blood pressure or protein in the urine may indicate kidney involvement.
- Untreated PAN can lead to renal artery damage and reduced kidney function.
- Immunosuppressive drugs combined with blood pressure control are essential to protect kidney health.
3. Nervous System
- Peripheral neuropathy, numbness, or weakness in hands and feet due to nerve damage.
- Severe cases may involve strokes or brain hemorrhages if major vessels are affected.
- Tailored therapy focuses on reducing inflammation, protecting nerves, and preventing long-term disability.
4. Gastrointestinal System
- Abdominal pain, ulcers, or intestinal bleeding may occur from reduced blood flow.
- PAN affecting the gut requires prompt diagnosis to prevent perforation or obstruction.
- Aggressive treatment, nutritional support, and sometimes surgical intervention may be needed.
5. Heart and Major Vessels
- Rarely, PAN can affect the coronary or large arteries, leading to serious complications.
- Symptoms like chest pain or shortness of breath must be evaluated immediately.
- Cardiac imaging and specialized vascular care are critical for these patients.
At IRIS Clinics, treatment for PAN is highly individualized. First-line therapy usually involves high-dose corticosteroids to quickly reduce inflammation. In more severe cases, immunosuppressive agents like cyclophosphamide, azathioprine, or methotrexate are added. For patients with hepatitis B-associated PAN, antiviral therapy is integrated into care plans. Lifestyle adjustments, physical rehabilitation, and regular monitoring ensure patients can manage side effects and maintain quality of life.
Long-term care involves preventing relapses and monitoring organ health. Routine imaging, blood pressure checks, and laboratory tests are vital for detecting early signs of recurrence. Patient education is a core part of our program—helping individuals understand medication schedules, warning signs of flare-ups, and the importance of consistent follow-up visits. At IRIS Clinics, our goal is not just disease control but supporting patients in achieving long-term wellness and improved daily function.