Polyarteritis Nodosa: Rare Vasculitis Symptoms and Diagnosis Explained
Polyarteritis Nodosa (PAN) is a rare but serious autoimmune condition characterized by inflammation of medium-sized arteries. This inflammation causes the blood vessel walls to weaken, leading to reduced blood flow and damage to the organs and tissues they supply. At IRIS Clinics, we often emphasize that early detection of PAN is crucial because delayed diagnosis can lead to complications involving the skin, kidneys, nerves, and gastrointestinal tract. Recognizing symptoms early allows for timely treatment, preventing long-term damage and improving outcomes.
Unlike common arthritic or inflammatory conditions, PAN is not triggered by joint overuse or aging. It results from an abnormal immune response, where the body mistakenly attacks its own arteries. This autoimmune reaction leads to vessel wall inflammation, narrowing, and sometimes aneurysm formation. Without treatment, these changes can restrict blood flow to vital organs, causing pain, tissue damage, and potentially life-threatening complications.
Understanding the hallmark signs of Polyarteritis Nodosa is essential. At IRIS Clinics, our rheumatology and vascular specialists utilize advanced diagnostic tools, including blood tests, imaging, and tissue biopsies, to identify PAN early and customize treatment plans for each patient.
The symptoms of PAN are often wide-ranging and may mimic other conditions, making diagnosis challenging. Patients may initially present with unexplained fatigue, muscle or joint pain, weight loss, and persistent fever. Other warning signs include skin lesions, nerve pain, or abdominal discomfort due to compromised blood supply. Because PAN affects arteries throughout the body, symptoms vary depending on which organs are involved, making comprehensive evaluation critical.
At IRIS Clinics, we recommend prompt consultation if patients experience ongoing, unexplained symptoms. Our multidisciplinary approach includes laboratory workups for inflammation markers, ANCA testing (though often negative in PAN), angiography to detect vessel abnormalities, and targeted biopsies. Early diagnosis allows for treatment before irreversible damage occurs.
Common Symptoms and Organ Involvement in PAN
Here’s how PAN typically manifests in different parts of the body and the symptoms to watch for:
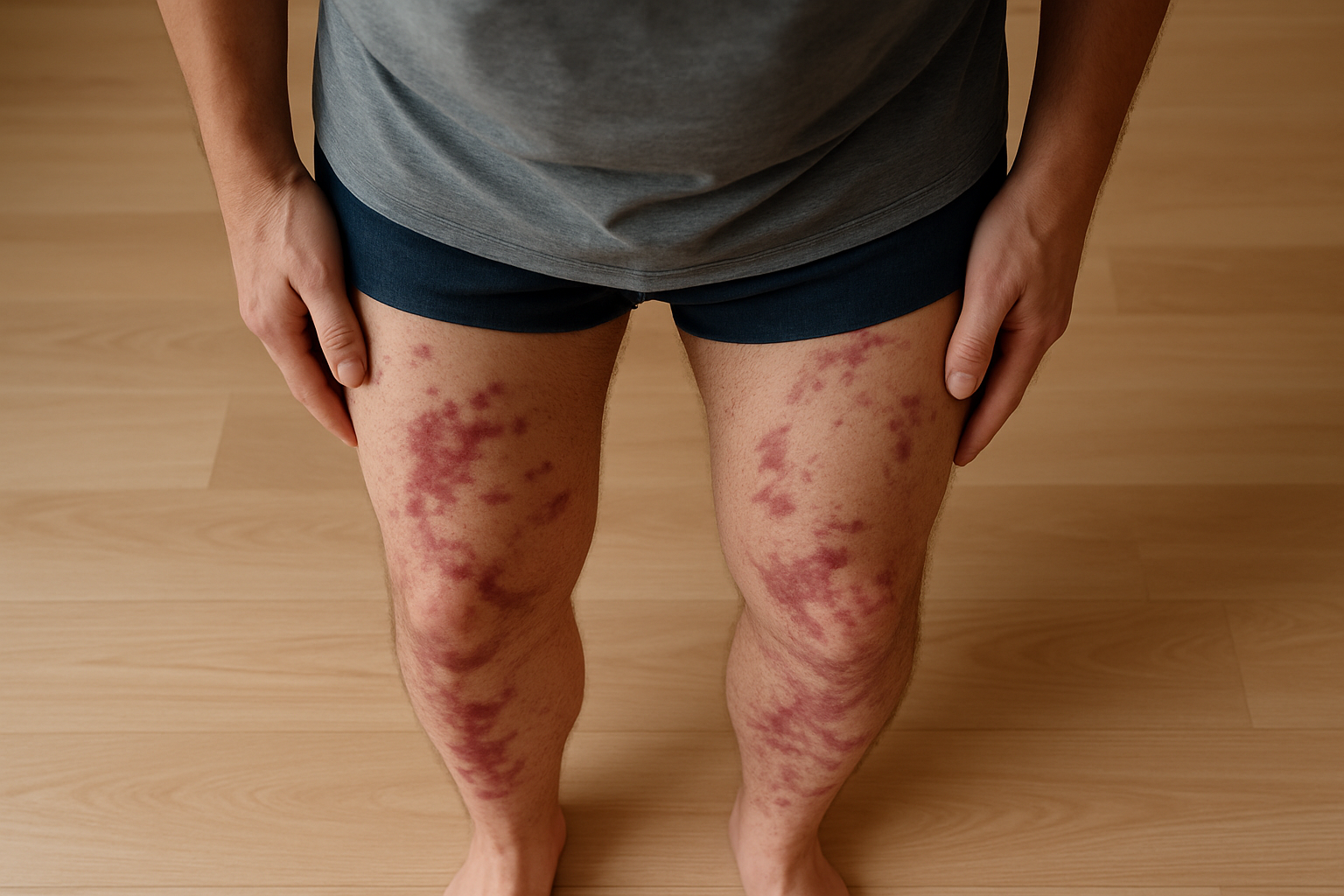
1. Skin and Peripheral Nerves
- Painful skin nodules or purplish patches (livedo reticularis).
- Ulcers or gangrene in severe cases due to compromised blood flow.
- Nerve pain, numbness, or weakness, often in hands or feet (mononeuritis multiplex).
2. Kidneys and Blood Pressure
- High blood pressure resulting from narrowed renal arteries.
- Kidney function decline or evidence of protein or blood in urine.
- Left untreated, may lead to chronic kidney disease.
3. Gastrointestinal Tract
- Abdominal pain after eating due to reduced intestinal blood flow.
- Possible nausea, vomiting, or blood in stool.
- Severe cases can cause intestinal perforation or bleeding.
4. Muscles and Joints
- Generalized muscle aches and joint pain.
- Weakness and stiffness that can limit mobility.
- Often mistaken for arthritis or fibromyalgia in early stages.
5. Other Organs and Systemic Signs
- Heart: Rare but possible involvement can lead to chest pain or heart failure.
- Nervous System: Stroke-like symptoms or nerve damage in severe cases.
- Constitutional symptoms: Ongoing fever, night sweats, fatigue, and weight loss.
Treatment at IRIS Clinics focuses on reducing inflammation, protecting organs, and improving quality of life. PAN management typically involves corticosteroids to control inflammation, immunosuppressive medications like cyclophosphamide or azathioprine for long-term control, and supportive therapies such as blood pressure regulation and physiotherapy. Each plan is individualized to the patient’s organ involvement and disease activity. Follow-up care, regular monitoring with imaging and labs, and patient education are essential components to prevent relapses and complications.
Because PAN is rare, awareness is critical. IRIS Clinics remains committed to improving outcomes through early recognition, advanced diagnostics, and multidisciplinary care, helping patients lead fuller, healthier lives despite this challenging condition.